Diabetic Retinopathy: Causes, Symptoms, and Treatment
Diabetic retinopathy is a serious eye condition that can occur in people with diabetes
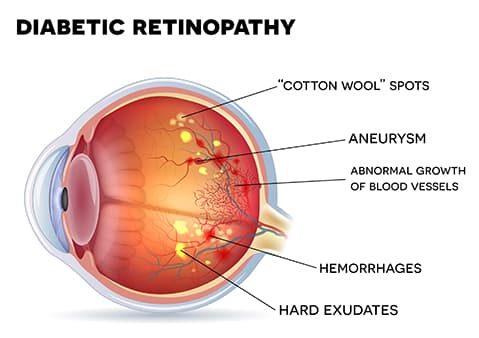
Diabetic retinopathy is a serious eye condition that can occur in people with diabetes. It affects the blood vessels in the retina, the light-sensitive tissue at the back of the eye, and is one of the leading causes of blindness in adults. Early detection and treatment are crucial to prevent or slow the progression of this condition. This article will provide an overview of diabetic retinopathy, including its causes, symptoms, stages, and treatment options.
What is Diabetic Retinopathy?
Diabetic retinopathy is a complication of diabetes that damages the blood vessels in the retina. These blood vessels can leak fluid or hemorrhage, leading to vision impairment or even blindness if not managed appropriately. The condition typically affects both eyes and progresses over time, making regular eye exams essential for people with diabetes.
Causes of Diabetic Retinopathy
Diabetic retinopathy is caused by prolonged high blood sugar levels, which can damage the blood vessels in the retina. Several factors can increase the risk of developing diabetic retinopathy, including:
- Duration of Diabetes: The longer a person has diabetes, the higher the risk of developing diabetic retinopathy.
- Poor Blood Sugar Control: Consistently high blood sugar levels can accelerate the damage to retinal blood vessels.
- High Blood Pressure: Hypertension can exacerbate the damage to the retinal blood vessels.
- High Cholesterol Levels: Elevated cholesterol can contribute to blood vessel damage and increase the risk of diabetic retinopathy.
- Smoking: Smoking can impair blood circulation and increase the risk of diabetic complications, including retinopathy.
- Pregnancy: Pregnancy can sometimes worsen diabetic retinopathy, making close monitoring necessary for pregnant women with diabetes.
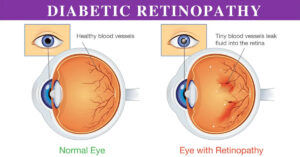
Symptoms of Diabetic Retinopathy
In the early stages, diabetic retinopathy may not cause any noticeable symptoms. As the condition progresses, symptoms may include:
- Blurred Vision: Vision may become blurry, making it difficult to read or perform other tasks that require clear vision.
- Floaters: Small dark spots or strings (floaters) may appear in the field of vision.
- Impaired Color Vision: Colors may appear faded or less vibrant.
- Dark or Empty Areas in Vision: There may be dark spots or empty areas in the visual field.
- Vision Loss: In advanced stages, diabetic retinopathy can lead to significant vision loss or blindness.
Stages of Diabetic Retinopathy
Diabetic retinopathy is classified into four stages, based on the severity of the damage to the retina:
- Mild Non-Proliferative Retinopathy:
- This early stage is characterized by small areas of swelling in the retinal blood vessels. Tiny, balloon-like bulges, known as microaneurysms, form in the blood vessels, which may leak fluid into the retina.
- Moderate Non-Proliferative Retinopathy:
- As the disease progresses, blood vessels in the retina become blocked, restricting blood flow and causing damage to the retina.
- Severe Non-Proliferative Retinopathy:
- More blood vessels become blocked, depriving several areas of the retina of their blood supply. The retina sends signals to the body to grow new blood vessels in response to this damage.
- Proliferative Diabetic Retinopathy:
- In the most advanced stage, new blood vessels begin to grow in the retina. These new blood vessels are abnormal and fragile, often leading to severe vision problems. They can leak blood into the vitreous (the gel-like substance that fills the center of the eye), causing severe vision loss and potentially leading to retinal detachment.
Diagnosing Diabetic Retinopathy
Diabetic retinopathy is typically diagnosed through a comprehensive eye examination. Key diagnostic tests include:
- Dilated Eye Exam:
- During this exam, drops are placed in the eyes to dilate (widen) the pupils, allowing the eye doctor to examine the retina and blood vessels for signs of damage.
- Fluorescein Angiography:
- A special dye is injected into a vein in the arm, and images of the retina are taken as the dye circulates through the retinal blood vessels. This test helps identify any leaking blood vessels.
- Optical Coherence Tomography (OCT):
- This imaging test provides detailed cross-sectional images of the retina, allowing the eye doctor to detect swelling, fluid accumulation, or other changes in the retinal tissue.
Treatment Options for Diabetic Retinopathy
The treatment of diabetic retinopathy depends on the stage of the disease and the severity of the symptoms. Treatment options may include:
- Managing Diabetes:
- The most important step in preventing or slowing the progression of diabetic retinopathy is to manage blood sugar levels, blood pressure, and cholesterol levels effectively. This may involve lifestyle changes, medications, and regular monitoring of blood glucose levels.
- Laser Treatment (Photocoagulation):
- Laser surgery can be used to shrink or seal leaking blood vessels in the retina. This treatment is particularly effective in the early stages of diabetic retinopathy and can help prevent vision loss.
- Injections:
- Anti-VEGF (vascular endothelial growth factor) medications, such as Avastin, Lucentis, or Eylea, can be injected into the eye to reduce swelling and prevent the growth of abnormal blood vessels. Steroid injections may also be used in some cases.
- Vitrectomy:
- In advanced cases where there is significant bleeding into the vitreous or retinal detachment, a surgical procedure called vitrectomy may be necessary. This procedure involves removing the vitreous gel and replacing it with a saline solution to restore clear vision.
- Regular Eye Exams:
- Regular eye exams are crucial for detecting diabetic retinopathy early and monitoring the progression of the disease. Early detection can lead to timely treatment and better outcomes.
Preventing Diabetic Retinopathy
While it may not be possible to prevent diabetic retinopathy entirely, there are steps you can take to reduce the risk and slow its progression:
- Control Blood Sugar Levels: Maintaining blood sugar levels within the target range can significantly reduce the risk of diabetic retinopathy.
- Monitor Blood Pressure and Cholesterol: Keeping blood pressure and cholesterol levels under control can help protect the blood vessels in the retina.
- Quit Smoking: Smoking can increase the risk of diabetic complications, including retinopathy. Quitting smoking can improve overall eye health.
- Regular Eye Check-Ups: Schedule regular eye exams, even if you don’t notice any vision problems. Early detection is key to preventing vision loss.
- Healthy Lifestyle: Adopting a healthy diet, exercising regularly, and managing stress can all contribute to better diabetes management and reduce the risk of complications.
Conclusion
Diabetic retinopathy is a serious complication of diabetes that can lead to vision loss if not managed properly. Understanding the risk factors, recognizing the symptoms, and seeking regular eye care are essential steps in protecting your vision. If you have diabetes, make sure to work closely with your healthcare team to manage your condition and schedule regular eye exams to detect any signs of diabetic retinopathy early.